Ovarian Rejuvenation with PRP Therapy
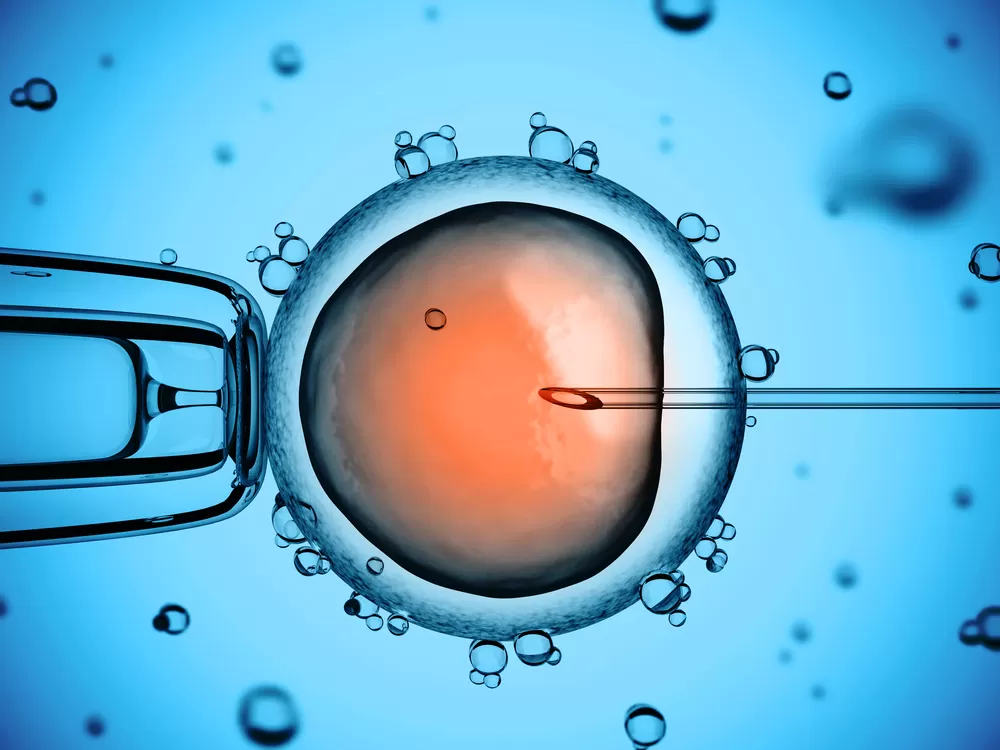
Ovarian rejuvenation is an advanced procedure that uses Platelet-Rich Plasma (PRP) to stimulate the ovaries, improve fertility, and increase the chances of pregnancy — either naturally or through assisted reproductive technologies such as IVF.
This method opens new possibilities for women experiencing decreased ovarian function or premature menopause.
Our Fertility Center was the first in Lithuania to introduce PRP therapy for ovarian stimulation.
How Does PRP Work?
Platelet-Rich Plasma (PRP) is a concentrated component of blood that contains a high level of growth factors and cytokines. When specially prepared PRP is injected into the ovaries, the growth factors help stimulate ovarian stem cells to regenerate and potentially form new egg cells.
Who Can Benefit from This Procedure?
- Women with low ovarian reserve and reduced levels of Anti-Müllerian Hormone (AMH)
• Women undergoing IVF with diminished ovarian response
• Women in the perimenopausal phase who wish to conceive or improve their well-being without using hormone replacement therapy (HRT)
• Women who wish to delay the onset of menopause
Book a consultation — our doctor will assess your individual case and provide a clear, personalized recommendation.